It is well demonstrated that emotion enhances memory encoding and facilitates later recall.1
Such observations have important implications in the realm of psychopathology because many disorders have at their core an overly powerful emotional memory, often stemming from a negative life event.
For instance, in order for posttraumatic stress disorder (PTSD) to develop, one must experience a life threat accompanied by peritraumatic distress.2
During trauma exposure, endogenous stress hormones (i.e., noradrenaline) overconsolidate the traumatic memory.3
This memory is subsequently reactivated too easily by contextual cues, thereby eliciting strong conditioned emotional responses (PTSD, Hormones and Memory) as well as hyper-vigilance and avoidance of trauma reminders.
Numerous psychiatric disorders also have at their core a negative and sometimes traumatic emotional memory. Trauma exposure is known to increase the risk for other disorders, such as phobias, addiction, depression, panic disorder and obsessive–compulsive disorder. (PTSD in treatment resistant obsessive-compulsive disorder.)
Negative life events of lesser magnitude that occur during development or later are also believed to increase the risk for psychopathology. (The role of adversity and stress in psychopathology: some evidence and its implications for theory and research.)
Furthermore, addicted individuals feel unable to resist emotional memories of their past abuse, which manifest in the form of cue-elicited cravings and can contribute to relapse. (Experimental medicine in drug addiction: towards behavioral, cognitive and neurobiological biomarkers).
Thus, decreasing the grip of such powerful emotional memories would seem to have obvious therapeutic value for a whole class of disorders in psychiatry.
One way to decrease the influence of an emotional memory on behaviour would be to interfere with its consolidation, thereby leading to a degraded memory trace.
Memory consolidation refers to the time-dependent process of transferring new learning from short- to long-term memory storage where it is reputed to be permanent. (Carlson NR. Physiology of behavior. 10th ed. Boston (MA): Allyn & Bacon; 2010. Learning and memory; pp. 440–84)
In a landmark study, Cahill and colleagues (Propanolol effect on long term memory for an emotionally arousing short story) found that, compared with placebo, propranolol taken before viewing a set of emotionally disturbing slides prevented the heightened recall of those slides.
Since then, many studies have replicated this finding.
The robustness of this finding has been explored in a qualitative review paper, (Nordadrenergic modulation of working memory and emotional memory in humans) but has yet to be investigated by means of meta-analytic review.
In addition to replicating the results of Cahill and colleagues, several researchers have tried to extend them to memory reconsolidation.
Reconsolidation theory (Retrograde amnesia produced by electroconvulsive shock after reactivation of a consolidated memory trace) disputes the permanence of consolidated memories and posits that, in order to persist, a retrieved (i.e., recalled) memory needs to be saved again to long-term memory storage, thereby recapitulating, at least in part, the process of memory consolidation.
(Fear memories require protein synthesis in the amygdala for reconsolidation after retrieval. - LeDoux JE, Schafe GE, Nader K.)
From a therapeutic point of view, the advantages of blocking reconsolidation rather than consolidation are substantial, since it could allow the otherwise narrow window of opportunity for modifying unwanted memories to be opened at will. (Effect of post-retrieval propranolol on psychophysiologic responding during subsequent script-driven traumatic imagery in post-traumatic stress disorder.)
The substance most frequently used in humans to block memory consolidation and reconsolidation is propranolol.
Propranolol is a synthetic β-adrenergic receptor blocker that crosses the blood–brain barrier and exerts peripheral effects on the noradrenergic system as well as central (inhibitory) effects on protein synthesis.
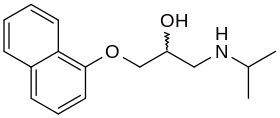
Pro·pran·o·lol prōˈpranlˌôl,-ˌäl/ noun.MEDICINE a synthetic compound that acts as a beta blocker and is used mainly in the treatment of cardiac arrhythmia.
(Attenuation of emotional and nonemotional memories after their reactivation: role of beta adrenergic receptors.
Impaired memory consolidation in rats produced with β-adrenergic blockade.
Memory for emotional material: a comparison of central versus peripheral beta blockade. J Psychopharmacol. 1999;13:32–9)
Protein synthesis is necessary to consolidate new learning to long-term memory storage. Animal studies have shown that infusing a protein synthesis inhibitor in the amygdala within the time-limited consolidation window leads to a subsequent memory impairment in a fear conditioning task.
(Protein synthesis and memory: a review. Psychol Bull. 1984;96:518–59.)
Protein synthesis is also required de novo for memory reconsolidation; postretrieval infusions of a protein synthesis inhibitor led to memory impairment of long-term memory, leaving short-term memory intact.
(Fear memories require protein synthesis in the amygdala for reconsolidation after retrieval.)
Propranolol is one of several protein synthesis inhibitors that have been used in animal studies to reduce the saliency of emotional memories.
(Fear memories require protein synthesis in the amygdala for reconsolidation after retrieval. Nature. 2000;406:722–6.)
Attenuation of emotional and nonemotional memories after their reactivation: role of beta adrenergic receptors.
(Impaired memory consolidation in rats produced with β-adrenergic blockade.)
A neuroimaging study revealed altered amygdala and hippocampus activity associated with propranolol-induced emotional memory impairment in healthy individuals. (Neural signature of reconsolidation impairments by propranolol in humans)
Propranolol is commonly used to treat migraine, tachycardia and performance anxiety.
(Propranolol in the management of recurrent migraine: a meta-analytic review.)
(Propranolol decreases tachycardia and improves symptoms in the postural tachycardia syndrome: Less is more)
(Effect of beta blockade and beta stimulation on stage fright.Am J Med)
It is also indicated as a second-line therapy for anxious states because of its effects on the noradrenergic system.
It reduces the flow of norepinephrine in certain parts of the brain.
Norepinephrine focuses your attention.
Going a bit further into the chemical train and there occurs a process of protein synthesis leading to the structure of long term memory.
So when you affect the flow of norepinephrine, ultimately you are affecting wether or not memories are consolidated which leads to the structure of long term memory.
Effecting the structure of long term memory through interventions that initiate memory reconsolidation can be epically transformative for clients that are seeking improvements in behaviours and overall life performance.